Have you ever noticed that what you eat impacts your mood? Have you felt worse after binging on junk food or after a night of drinking? There is compelling research suggesting that it may not be just the guilt talking - your microbiome may be contributing in a large way to the conversation.
What is the microbiome?
There are 10- to 100-trillion symbiotic microbes of various species existing in and around the human body, collectively referred to as the microbiome [1]. These friendly microbes outnumber your own human cells and have recently become popularized for the growing body of evidence detailing the vast impacts they have on human physiology and behaviour.
The microbes in your intestines make vitamins, amino acids, hormones, neurotransmitters and other signaling molecules that impact the way your brain and body function [2], [3]. They also produce short-chain fatty acids as byproducts that your intestinal cells use for energy, which contributes to healthy gut function [3].
These microbes live in our digestive tract and survive off the foods that we eat. Just like any other living organism, their health (and therefore ours) depends on consuming a healthy diet. It has been shown that dietary changes (e.g. from animal-based to plant-based), as well as any significant systemic stress and inflammation can alter the composition (i.e. diversity and abundance of species) of your microbiome within just 24 hours [3].
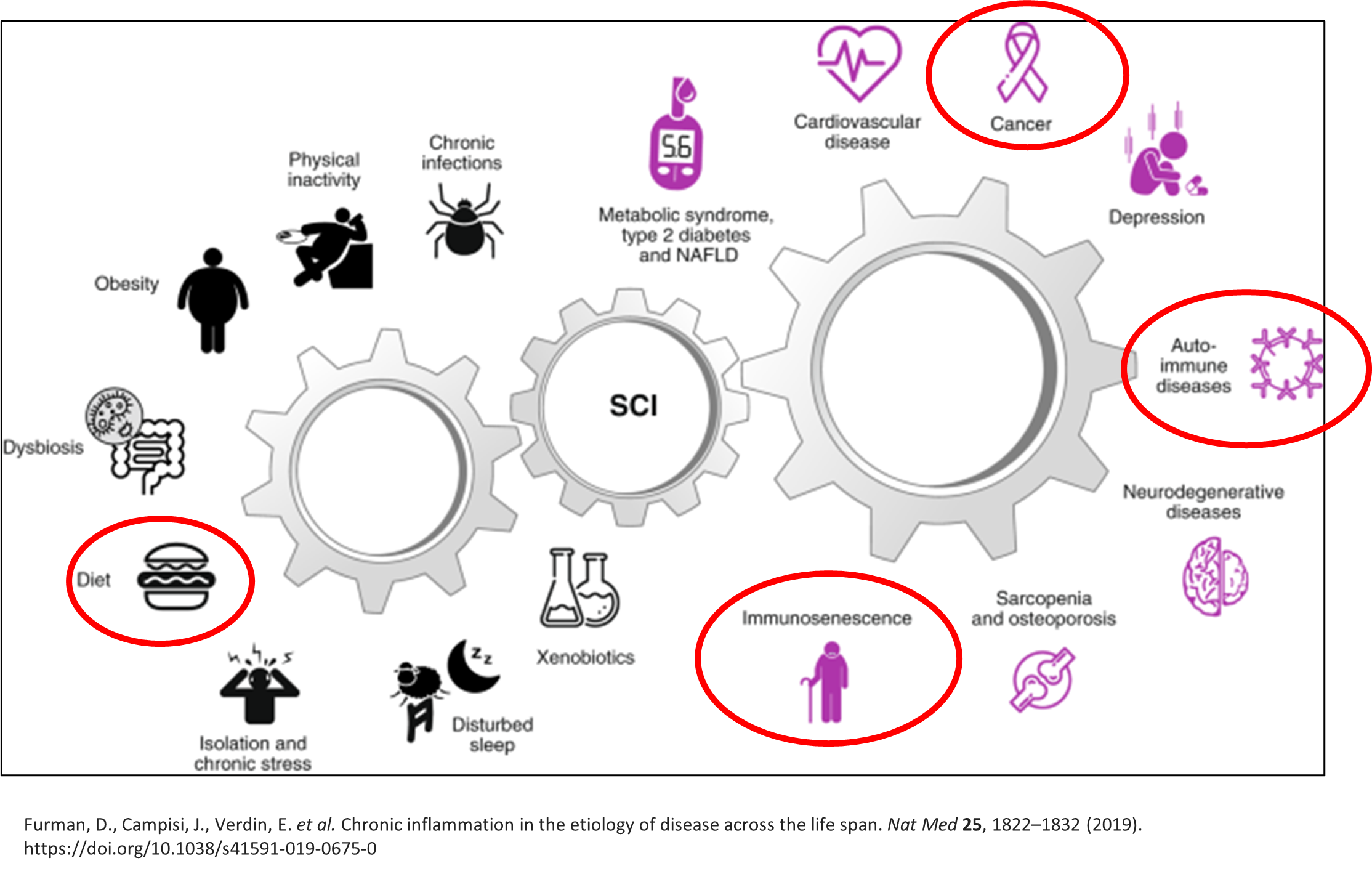
Altered microbiome composition has been associated with many conditions, such as inflammatory bowel disease (IBD), psoriasis, atopic dermatitis, autoimmune arthritis, type 2 diabetes, obesity, and atherosclerosis [3]. This is not surprising given the significant role these organisms have in regulating metabolism and immunity. In fact, researchers are finding that the microbiome composition in a given disease seem to have a different complement of microbes associated with it. For example, an IBD microbiome has less diversity (fewer species of healthy microbes), and lower numbers of good bacterial species. Therefore, it has lower short-chain fatty acid production [3]. Short-chain fatty acids (SCFAs) are essential to the health of your intestinal cells and are also thought to be anti-inflammatory in the gut [3].
The Microbiome’s Effect on Mood & Behaviour
Gut microbes relay messages to the brain via various direct and indirect mechanisms - bacterial metabolites, metabolic precursors, immune signalling, vagus nerve signalling, and Hypothalamic Pituitary-Adrenal axis activation [4], [5]. It is through these mechanisms that neurodevelopment or neurodegeneration are influenced [5]. A significant portion of the microbiome influence on the brain comes via the gut-brain axis: a bi-directional pathway connecting the nervous system in your digestive tract to the central nervous system (your brain) [4], [5]. As shown in the graphic below, your gut and your brain communicate directly via nerves that transmit different signals and molecules, which can have a profound effect both ways to both systems [6].
Photo credit: https://fhs.mcmaster.ca/forsythe-lab/microbiota_gut_brain_axis.html
Considering the gut-brain axis and the physical manifestations that different microbiome composition can produce, it should be no surprise that there are mental/emotional implications as well. Many psychiatric and neurological pathologies have gastrointestinal co-morbidities, including schizophrenia, autism, neurodegenerative diseases, anxiety, and depression [7]. As noted above, different pathologies have different microbiome composition. This extends to mood and neurodegenerative disorders, such as major depressive disorder, schizophrenia, Parkinson’s disease, and autism spectrum disorder [2], [5], [8]. There is also data suggesting that alterations in the microbiome from addictions (e.g. alcohol, cocaine) may be associated with substance cravings and increased risk of developing associated psychiatric disorders, such as anxiety and depression [9], [10].
Probiotics & Your Mood
Probiotics are supplements that contain healthy microbes that ,when ingested, influence the health of your microbiome. Probiotics used to benefit mood and cognition have been coined “psychobiotics,” and are a burgeoning new area of interest in research. A study by Tillisch et al. used brain scans (functional magnetic resonance imaging) to demonstrate the ability of probiotics to alter brain activity in areas associated with processing emotion and sensation, and to reduce negative thinking associated with sad mood [4], [7], [11], [12]. While most studies indicate that further research in this area is needed, associations between specific strains of microbial species and their benefits on various conditions are rapidly emerging [7], [13][14]. A recent human clinical trial of adjunctive probiotic intervention for Major Depressive Disorder (MDD) showed that compared with placebo, probiotic intervention exhibited greater improvement in depressive symptoms [15]. Participants who received the probiotic intervention experienced reductions in both depression and anxiety, and the probiotics were well-tolerated, prompting the authors to suggest probiotics as an acceptable adjunctive intervention for adults with MDD [15].
How Can I Support My Microbiome?
Lifestyle
A healthy lifestyle goes a long way in supporting your microbiome, and healthy eating is just one part of it. As mentioned earlier, dietary changes, significant systemic stress, and inflammation can alter your microbiome within just 24 hours. There are many different types of stress - physical, mental and emotional - that can lead to physiologic changes that can alter the microbiome. Practicing stress management through self-care, meditation, social connection, thoughtful schedule planning, getting adequate sleep, and setting appropriate boundaries with people and responsibilities will help you be more resilient in dealing with stress. The better you are at managing stress, the less likely it will spill over into added physical or mood-related symptoms.
Digestive Supports
Probiotics are a great start to improving your gut health and mood, though quality and potency matter! Our naturopathic doctors are here to assess if and which type of probiotics are most suitable for you, as well as to review if any further testing or treatments are indicated to optimize your digestive and mental health.
We are here to help, so reach out if you are looking for professional guidance!
In Health,
Dr. Jacalyn Sieben, ND
[1] Ursell, L.K. et al. (2012). Defining the human microbiome. Nutrition Reviews. Vol. 70 (Suppl. 1):S38- S44. doi:10.1111/j.1753-4887.2012.00493.x
[2] Dinan, T.G. & Cryan, J.F. Mood by microbe: Towards clinical translation. Genome Medicine. 8:36. DOI 10.1186/s13073-016-0292-1
[3] Corfe, B.M. et al. (2015). The multifactorial interplay of diet, the microbiome, and appetite control: current knowledge and future challenges. Proceedings of the Nutrition Society. 74, 235-244. doi:10.1017/S0029665114001670
[4] Dinan, T.G., Stilling, R.M., Stanton, C., Cryan, J.F. (2015). Collective unconscious: How gut microbes shape human behavior. Journal of Psychiatric Research. 63:1-9. http://dx.doi.org/10.1016/ j.jpsychires.2015.02.021
[5] Sharon, G. et al. (2016). The central nervous system and the gut microbiome. Cell. 167. http:// dx.doi.org/10.1016/j.cell.2016.10.027
[6] McMaster University. (2019). The microbiota-gut-brain axis. [Digital Image] Retrieved from: https:// fhs.mcmaster.ca/forsythe-lab/microbiota_gut_brain_axis.html
[7] Sampson, T.R. & Mazmanian, S.K. (2015). Control of brain development, function, and behavior by the microbiome. Cell Host & Microbe. http://dx.doi.org/10.1016/j.chom.2015.04.011
[8] Jiang, H. et al. (2015). Altered fecal microbiota composition in patients with major depressive disorder. Brain, Behavior, and Immunity. 48:186-194. http://dx.doi.org/10.1016/j.bbi.2015.03.016
[9] Hillemacher, T., et al. (2018). Alcohol, microbiome, and their effect on psychiatric disorders. Progress in Neuro-Psychopharmacology and Biological Psychiatry. Volume 85, Pages 105-115. https://doi.org/ 10.1016/j.pnpbp.2018.04.015
[10] Kiraly, D.D. et al. (2016). Alterations of the host microbiome affect behavioral responses to cocaine. Scientific Reports. 6:35455. DOI: 10.1038/srep35455
[11] Rea, K., Dinan, T.G., Cryan, J.F. (2016). The microbiome: A key regulator of stress and neuroinflammation. Neurobiology of Stress. 23-33. http://dx.doi.org/10.1016/j.ynstr.2016.03.001
[12] Tillisch, K., Labus, J., Kilpatrick, L., Jiang, Z., Stains, J., Ebrat, B., Guyonnet, D., Legrain-Raspaud, S., Trotin, B., Naliboff, B., et al. (2013). Consumption of fermented milk product with probiotic modulates brain activity. Gastroenter- ology 144, 1394–1401. DOI: https://doi.org/10.1053/j.gastro.2013.02.043
[13] Foster, J.A., Rinaman, L., & Cryan, J.F. (2017). Stress & the gut-brain axis: Regulation by the microbiome. Neurobiology of Stress. 124-136. http://dx.doi.org/10.1016/j.ynstr.2017.03.0 01
[14] Sarkar, A. et al. (2016). Psychobiotics and the manipulation of bacteria-gut-brain signals. Trends in Neurosciences. Vol 39, No. 11. http://dx.doi.org/10.1016/j.tins.2016.09.002
[15] Nikolova VL, Cleare AJ, Young AH, Stone JM. (2023). Acceptability, Tolerability, and Estimates of Putative Treatment Effects of Probiotics as Adjunctive Treatment in Patients with Depression: A Randomized Clinical Trial. JAMA Psychiatry. doi:10.1001/jamapsychiatry.2023.1817